If you’ve never heard of the connective tissue disorder systemic sclerosis before, you’re not alone. That’s because fewer than 5,000 cases of the extremely rare autoimmune disease – for which there is no cure – are diagnosed each year. But while systemic sclerosis isn’t exactly a household name, the low number of cases should never underscore the severity of this debilitating and sometimes fatal illness.
Systemic sclerosis affects the connective tissue of the body in two ways. The first type of systemic sclerosis is considered “localized,” meaning it only appears externally, usually on the hands, feet, arms, legs and face. Localized systemic sclerosis causes the affected skin to accumulate excess collagen, which in turn appears as a thickening of the skin in those areas.
“Systematic” systemic sclerosis develops inside the body, causing a thickening or hardening of tissue on the lungs, heart, kidneys and gastrointestinal tract.
But while both types of systemic sclerosis can be painful and even embarrassing, systematic systemic sclerosis can cause everything from pulmonary hypertension to some forms of cancer to other fatal conditions caused by the hardening of tissue. But now, researchers say systemic sclerosis could cause yet another painful condition: temporomandibular joint (or TMJ) disorder.
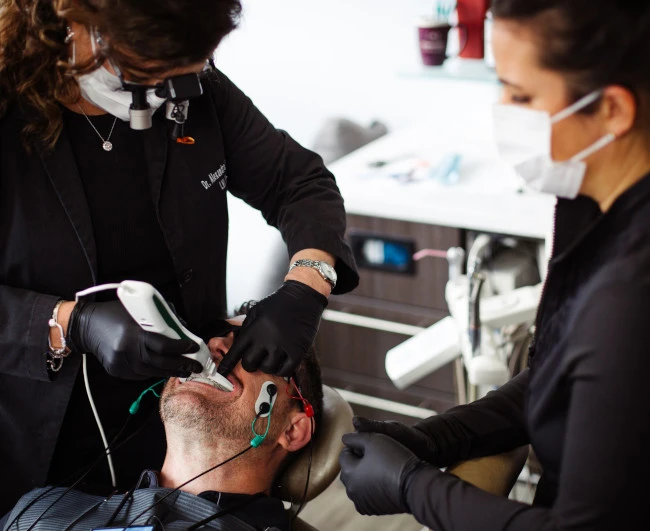
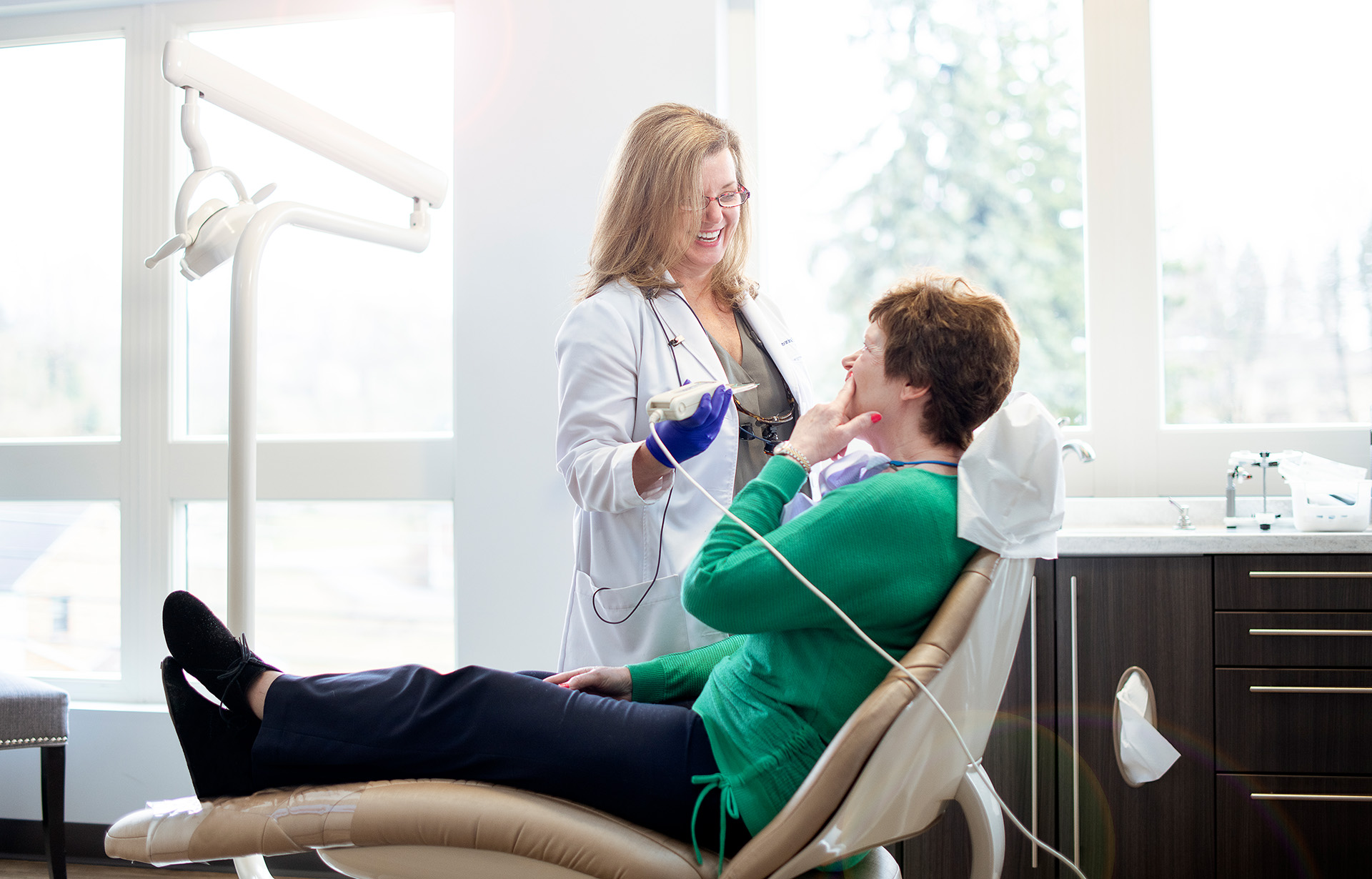
Dr. Alexandra George treats patients with temporomandibular joint disorder in her Wexford, Pennsylvania, dental clinic. She says the link between systematic sclerosis and TMJ disorder makes a lot of sense.
“The temporomandibular joint is surrounded by muscles that we use to chew, talk and basically move our mandibles the way they should,” George says. “Those muscles in turn are covered by something called fascia, which is connective tissue. That fascia is what’s responsible for much of the myofascial pain patients report with TMJ disorder. It also happens to be the very thing affected by systemic sclerosis.”
The study was presented at a recent European League Against Rheumatism (EULAR) conference and revealed that patients with systemic sclerosis were more likely to develop TMJ disorders than those in a control group. They were also more likely to have TMJ disorder symptoms including the “clicking and popping” of the jaw commonly associated with TMJ disorder, as well as more jaw pain than those in the control group. Not surprisingly, the TMJ pain increased concurrently with the severity of the systemic sclerosis. But while not every systemic sclerosis patient will develop TMJ disorder, nor does every TMJ disorder sufferer have systemic sclerosis, George believes the study’s findings still reveal an important truth.
“What this tells me as a doctor is that we need to screen systemic sclerosis patients early and regularly for TMJ disorders. Many patients have found tremendous relief from TMJ disorder pain with neuromuscular dentistry,” says George. “We may not be able to cure either condition yet, but if we work together we can help ease some of the suffering these patients endure with both conditions.”